by Alexandra Godfrey, PA-C
 Guatemalan Village
Guatemalan Village
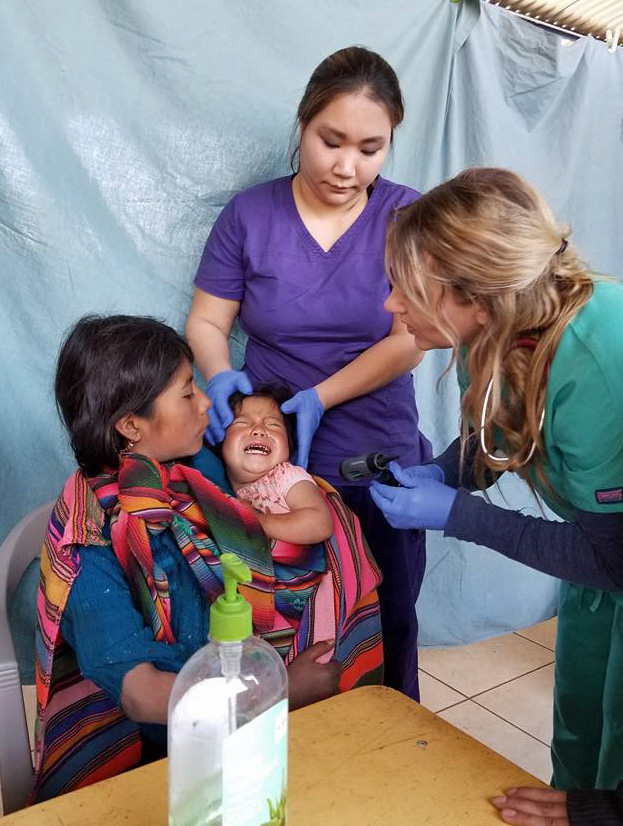
The child lies across her mother’s lap. Her eyes are hollow, and I hear the rattle of her breathing. She’s tachypneic, tachycardic, and febrile. Her right lung wheezes and crackles, and her tongue sticks to the roof of her mouth. Her name is Elisa. She is four years old.
Elisa sustained a traumatic brain injury in a car accident when she was two years old. Now she can neither walk nor speak. She has struggled with multiple illnesses, and this time her family cannot get her to eat or drink. Without aggressive intervention, I think Elisa might die. I want to transfer her to the hospital for a higher level of care. This would be an easy decision in America. However, today I am not in America. And the usual rules do not apply.
 Clinic room in Guatemala
Clinic room in Guatemala
I am working as a PA in a pop-up clinic in the remote mountain village of Paraxquim in western Guatemala. The road to the village is a track winding steeply up the mountainside along a precipitous drop. Trash litters the roadside, and the pungent smell of rotten debris on the rugged climb made two of our team vomit. We created our clinic in the village hall. Clothes pegs, drapes, and string make up our “rooms.” We examine patients on school desks placed end to end, their heads on ink wells and their feet against the wall. We lack access to labs, imaging or specialist services. We have medicines, the usual equipment for vital signs and ourselves. I have already splinted a fracture using tongue blades, bandages and tape and sent a man with angina home with lisinopril, aspirin, and a prayer.
A septic child? I felt a tightness in my chest and a sinking feeling in my stomach. To transfer Elisa from the clinic, we would need to use our own vehicle and leave some of our team behind. The hospital is hours away. Would she even make the journey?
At the hospital, the family would need to pay upfront: initial evaluation, lab work, X-rays, medicines, time in the hospital. Guatemala’s Constitution supports healthcare for all, but government funding is among the lowest in the world, and close to half the population has no access to care, struggling with pneumonia, heart disease, intestinal parasites, malnutrition, inadequate housing, and poor sanitation. Elisa’s family lives in a hut with a dirt floor on around $10 per week. Either we transport the child using our own limited funds to pay for her care and leaving the remaining villagers to fend for themselves, or we treat her here knowing that she might not survive.
I initiate care. I give Elisa Zofran, Tylenol, fluids and our only gram of ceftriaxone. I ask her family to stay with us in the clinic so we can monitor her progress. About mid-day, an experienced paramedic on our team approaches me. He wants to talk about Elisa. He rubs his forehead, then opens and closes his mouth as though struggling:
“If we use all our resources on Elisa, what happens to those we won’t be able to treat? What quality of life can this child expect, at best?”
He’s an amazing clinician and educator, and I appreciate his questions. Still, I sense that I am being asked to make value judgments on a life. I have a child with a severe and chronic illness myself, so this touches me personally. I, too, have faced my child’s mortality. I wonder if anyone ever questions my child’s value. My instinct is to treat Elisa as I would my own. But she isn’t my own. We aren’t in America. This isn’t my family. I must consider not only the best interests of this child, but also the team and community. I think we all have life experiences that make us particularly sensitive to a particular condition or presentation. And I recall the advice from my first job in emergency department:
“Alex, remember while you are giving everything to one patient, someone else in the waiting room might end up with nothing.”
I check on Elisa often. I note that her temperature is coming down. Her breathing improves, and by the end of the day she starts to tolerate oral fluids. This is a real breakthrough. As the day draws to a close, her vitals have all returned to normal. She is still very sick, but she looks much better. I tell the team that Elisa might be okay if we supply her family with antibiotics, anti-pyretics, Albuterol, anti-emetics, Pedialyte and some sort of nutrition. I think the journey to the hospital might pose a bigger risk to her and her family. Part of me wants the others to question my judgment. But they don’t. Their trust astounds me.
I look at Elisa sleeping comfortably on her mother’s lap. I think, better to die here in the safety of your mother’s arms than in a strange and distant place.
We leave the village that evening. We will never know whether or not Elisa survives the night.